In just the past two months since the coronavirus began sweeping across the United States, telemedicine—oftentimes referred to by the more uplifting moniker of telehealth—has emerged as one of the most explosive sectors within the U.S. economy.
Widespread shelter-in-place orders have forced many consumers to forgo or delay most discretionary services (a haircut can wait, as well as a regular dental checkup and cleaning), but despite mounting evidence that some patients with critical needs are delaying important health care decisions that require hospital visits, the general population’s need for non-elective health care services has not dissipated. To meet baseline demand, in addition to marshaling additional resources for dealing with the onslaught of COVID-19 cases, physicians and hospital systems are increasingly turning to a network of technology-enabled digital telehealth solutions to bridge the gap.
Some of these solutions are as simple as providing a platform for doctors to conduct secure, virtual consultations with patients in the safe social-distancing environs of their own living rooms—something akin to a Zoom call with a physician. Other solutions are far more sophisticated, such as using artificial intelligence (AI) to deliver asynchronous content to dynamic platforms, which enables both physicians and patients to connect while saving time and money for both parties.

Meanwhile, a mishmash of government leaders, public health authorities, insurers and hospital systems have been scrambling to stitch together a viable framework to deliver as many traditional health care services as possible online. These efforts—despite being hampered by an astonishing lack of centralized coordination—are nonetheless proving to be a boon for the companies playing in the broader telehealth and telemedicine sandbox. The companies in this space, comprised mainly of digital health startups whose DNA is equal parts health care and technology, provide a panoply of distance and remote services for patients, hospital systems, physicians, laboratories, pharmacies and other key constituencies in the health care delivery ecosystem.
“This toothpaste is not going back into the tube. Telehealth will be the new normal after the coronavirus pandemic subsides.”
“The dirty little secret that any physician who is being honest will tell you is that 90 percent of primary care visits can be done remotely—the ‘in-person’ part just makes the patients feel better because they are able to look their doctor in the eye,” said Alex Turkeltaub, founder of Roam Analytics, a San Francisco-based health care analytics company. “The reality is that the tools for remote doctor visits have been in place for a while and only now—because COVID-19 is forcing them to do so—are providers, insurance companies and regulators lining up to leverage the technologies that are out there.”
“But once everyone in the system gets exposed to the benefits and efficiencies of telehealth, it will become the dominant way to access primary care. Shortages of doctors, particularly in rural areas, can be alleviated quickly via telehealth,” added Turkeltaub, who is now setting up a health care investment firm looking to seize upon new opportunities opening up across health care in a post-COVID-19 world.

“Prior to this pandemic, telehealth never experienced mass consumer adoption,” remarked Taqee Khaled, head of strategy at digital consultancy Nerdery, in a recent interview with MobiHealthNews. His company works with U.S. provider networks on their digital and telehealth offerings. “The pandemic has changed all of that in an instant. Regardless of who was ready to provide telehealth, social distancing policies in effect mean that 100 percent of the population requires a telehealth option as the first point of contact.”
For One Telehealth Company, COVID-19 Is ‘Make or Break’
Perhaps the best known company in the booming consumer telehealth space is Teladoc Health, a global telemedicine and virtual health care conglomerate founded in Dallas, Texas in 2002. Company shares have shot up over 50 percent in the past three months, but surging consumer demand is proving to be the company’s ultimate test.
Well-funded from the beginning, the company used plenteous venture capital to vacuum up a handful of its biggest competitors on its way to a 2015 IPO on the New York Stock Exchange. Yet, despite its early successes, since going public, the company has seemingly careened from one scandal to another as it has struggled to integrate its acquisitions and upgrade its technology from its call-center DNA.
Teladoc Health faced a great deal of opprobrium for several incidences in recent years, the most egregious being a 2018 episode in which the company’s CFO and COO Mark Hirschhorn was ousted amidst allegations of sexual misconduct and insider trading, which resulted in a class action lawsuit. Some health care insiders privately suggest that Teladoc, although pioneering the telehealth industry, has really been the result of savvy financial engineering, not breakthrough technology or health care delivery innovation. Many telehealth executives believe that the company had essentially stymied the sector’s evolution by crowding out, or buying up, the competition.
Washington Is Actively Encouraging Adoption of Telehealth
Whether or not Teladoc Health’s cunning business acumen or high-profile missteps kept the sector from going more mainstream earlier is still open to debate, but now, with state and local authorities across the country reeling in light of the pandemic, supporting telehealth is currently an imperative in Washington, D.C.
This past week, the Federal Communications Commission (FCC) announced a new $200 million program to help fund telehealth initiatives for qualifying providers during the COVID-19 pandemic. The program, which taps into the Federal Government’s Coronavirus Aid, Relief and Economic Security (CARES) Act, aims to jumpstart telemedicine programs across the country in an effort to drive efficiencies across the health care system, freeing up as much physical space in clinics and hospitals as possible so that valuable health care resources are directed to those most in need. This initiative comes on the heels of comments by Dr. Nancy Messonnier, the director of the CDC’s National Center for Immunization and Respiratory Diseases, who gave a full-throated endorsement of the sector, encouraging hospitals to look into expanding telehealth services to effectively offload some of their baseline demand.
“For years, archaic, complex and stifling regulations and rules from a mosh pit of oversights and special interests have kept health care locked in the 20th century,” commented Ethan Bearman, an on-air analyst with Fox Business Channel. “COVID-19 has changed all that. With stay-at-home orders across most of the country amid a raging global pandemic, the industry has had no choice but to finally embrace telehealth, and guess what—after COVID-19, there will be no going back. Distance medicine jumped ahead 25 years in the month of March here in the United States. And Washington understands that.”
Despite Washington’s renewed enthusiasm for distance medicine, across the country, fragmented state laws governing health insurance and reimbursement rules vary considerably and will force digital health companies to take a surgical approach in each jurisdiction. For example, a law passed in Iowa in 2018 orders insurance companies to provide coverage for telehealth, but it doesn’t require that telehealth visits be reimbursed at the same rate as in-person treatments, creating economic friction for hospital administrators looking to balance the books.
Demand for Telehealth Services Is Booming
Nonetheless, patients who are fearful of venturing out of their homes during the quarantine for routine doctor visits are turning to telehealth in droves.
Worth spoke with Jon Pearce, CEO of Minneapolis-based Zipnosis, a leading digital telehealth platform that has seen its volume of online consultations explode by an astonishing 3,600 percent over the past few weeks. “This toothpaste is not going back into the tube. Telehealth will be the new normal after the coronavirus pandemic subsides,” Pearce said.
“Consumers use their phones for just about everything, from ordering Domino’s pizza to checking a bank account balance. It’s a shame that up until now, many didn’t know they could use that same device to get health care,” he addded.

The trick, of course, is that these new platforms will have to work. “Traditional telemedicine has been plagued by some of the legacy issues dating back to its early days as call centers—that’s why it’s still called telehealth—but this epidemic is giving the entire sector an opportunity to really shine at a moment of nationwide need,” Pearce explained. “There will be lots of first-time users coming on board, and we must all work to make sure that their first experience is solid. A rising tide lifts all ships.”
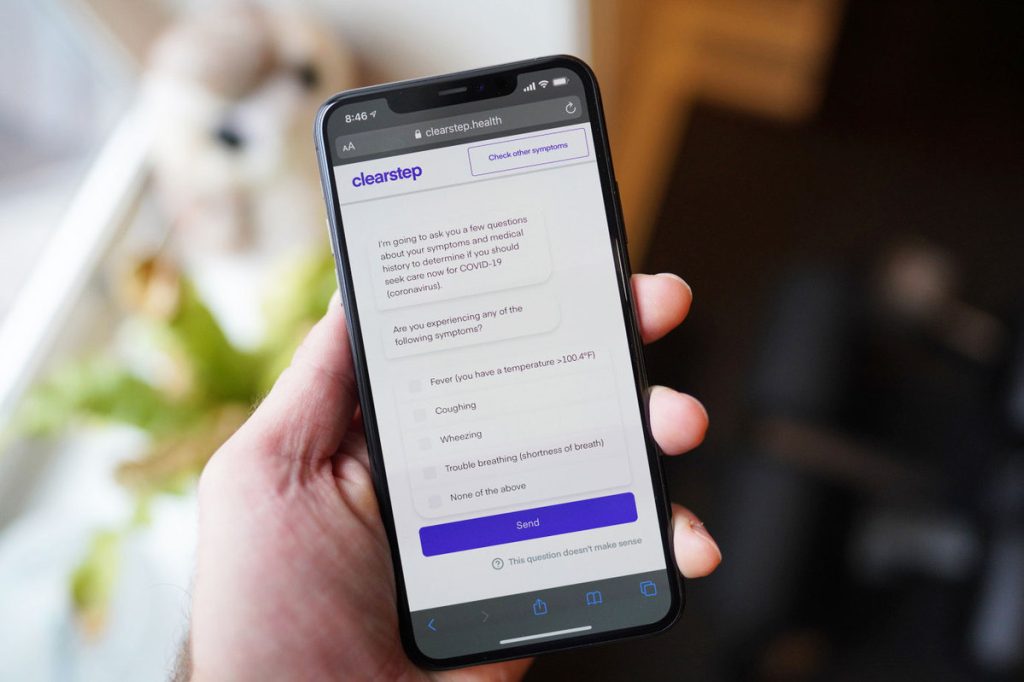
One mid-stage Chicago-based company has built an entire business model around patients’ all-important first step into the world of telehealth. Clearstep assists patients as they navigate their own unique health care journey, while helping health systems meet the demands of the modern consumer. With features such as AI-enabled symptom checking, it’s a platform that cracks open the door to truly bespoke telemedicine.
“Clearstep has been completely overhauling health care’s outdated user interface and customer experience. A user-friendly experience is especially important during the pandemic. People who are ill or anxious may not have the energy or patience to wade through a ton of text, links and information,” commented Clearstep cofounder and head of design Peter Garber. “The best solutions walk users step-by-step through their care options and address their concerns in a streamlined and individualized way.”
Another company that is riding the wave of increased sector-wide interest in telemedicine solutions is Vidscrip, a Minneapolis-based startup that enables physicians to record video answers to patients’ frequently asked questions, sharing them through channels they already use, like a doctor’s web page or SMS messages sent directly to patients’ phones. Vidscrip generally employs a sponsorship revenue model, ensuring that the service is always available to doctors free of charge.
The company recently announced a significant partnership with AstraZeneca to roll out the Vidscrip platform across the pharmaceutical giant’s network of hundreds of thousands of physicians nationwide to support messaging centered around COVID-19. The program aims to free up physician resources while helping patients make better and more informed decisions about their medical conditions and treatment plans as they relate to the novel coronavirus.
“There has never been a time when health care providers have had a greater need to stay connected to their patients and have less capacity to do so efficiently,” said John Brownlee, CEO and cofounder of Vidscrip. “Our technology platform is perfectly positioned to ensure that patients get the right information, at the right time, from their own trusted care team.”
“Distance medicine jumped ahead 25 years in the month of March here in the United States. And Washington understands that.”
For the medical community, acceptance of telehealth solutions, like Zipnosis, Clearstep and Vidscrip, across the health care ecosystem is long overdue.
“We don’t adopt technologies to share patient-centric information, but we are quick—perhaps too quick—to adopt new technologies for clinical reasons. Now, all that is beginning to change,” observed Dr. Howard Luks, an orthopedic surgeon based in Westchester County, just outside of New York City. “Companies like Vidscrip are playing a really transformative role in driving efficiency, so doctors can spend more time being doctors and less time repeating the same exact information over and over—information patients usually won’t retain much of anyway. This technology delivers physician information to patients in a format they can review and rewind as much as needed.”
“It saves me and my administrative staff from countless hours of playing phone tag and fielding calls from people who didn’t retain much of the information I initially shared. Overall, it’s a huge time saver, and it’s really improved my office efficiency. My patients are better informed,” Luks added.
COVID-19 will permanently alter many aspects of American daily life. It is still too early to tell how the pandemic will affect schools and business as they begin to reopen, or the service industry as it attempts to get back on its feet. But this much is clear already: The current pandemic will upend how we think about health care, as telehealth and telemedicine become integral, sine qua non components of the U.S. health care delivery system.







